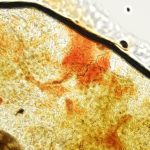
Atopic dermatitis: Which clinical signs can be found and how to diagnose it?
Diagnosis of allergy is always clinical, is based on the data obtained from the anamnesis (including age, breed, seasonality) and the clinical examination.
Allergy tests are necessary to identify the allergens to which the animal is sensitive and is required to carry out allergen-specific immunotherapy (ASIT or hyposensitization treatment).
The main allergens are dust and storage mites; grass, plant and tree pollen; fungal spores, also fleas in dogs and cats and insects in horses.
In dogs, atopic dermatitis is the second most common non-infectious disease. It appears commonly between six months and three years of age, but can develop at any age and manifests itself with pruritus and associated characteristic cutaneous clinical signs (primary pruritus, sine materia).
The clinical picture in the cat is more similar to that of horses than of dogs. It can present with clinical respiratory signs such as feline allergic bronchitis, asthma and rhinitis. However, skin lesions, as self-induced alopecia, excoriations and ulceration, miliary dermatitis and other injuries of the eosinophilic granuloma complex are the most frequent clinical signs.
When is the ideal time to perform allergy tests?
In case of seasonal allergies, ideally, they should be carried out towards the beginning or shortly before the end of the season.
When seasonal clinical signs begin wait one month before carrying out allergy tests.
In the case of perennial allergies, which do not show seasonality, allergen tests can be carried out at any time of the year.
Is it possible to send other material besides serum to carry out the allergy tests?
For determining of antibodies serum is always preferable. Allergy tests are mainly validated using serum, however it is possible to perform them from blood preserved in tubes with heparin or EDTA.
How long can a blood sample be kept for allergy testing in the fridge or freezer?
Antibodies are well preserved in frozen samples for long periods, there would be no problem in performing the analysis even on samples kept for up to one year. But after this period of time the results may not correspond to the current state of sensitisation of the animal, so an updated sample would be recommended.
For samples that have been refrigerated (8-10ºC) the antibody study should be carried out within four weeks from collection.
Screening test: Is it necessary to do it, or can main panel tests be done directly?
It is not obligatory to perform the allergy screening test (pre-test or group test) before the main panels.
With a clear clinical picture of allergy, you can begin with the main allergy panels (Mediterranean, insects, Nordic, annual and seasonal panels). With positive results, the allergen-specific immunotherapy treatment (ASIT) can be ordered immediately, saving the cost of the screening test.
Nevertheless, in many other cases, screening may be the most cost-effective option before entering the field of allergen differentiation, for example:
– If the animal is only positive to one of the groups, the cost of the differentiation of the other tests can be saved.
– In the case of animals that have been controlled with cortisone and the withdraw times could not be respected, the screening
test verifies that the identification of antibodies is possible, without making a more significant investment in the differentiation
panels.
– There are animals that, although atopic, can give negatives in the allergen measurement tests. In these cases, it saves on the
cost of the differentiation panels.
– In seasonal allergies, it can help determine the right time of year for differentiation.
– The pre-screening test also has the great advantage that it includes the measurement of antibodies against fleas.
Positive screening test: why test for differentiation of allergens? Why not do a standard ASIT for annual or seasonal allergens?
Each animal, like people, reacts individually to different allergens. Studies show that using a „standard“ ASIT with the most common year-round or seasonal allergens has much lower success rates (30%, placebo) than a solution tailored to each patient.
Therefore, the individual differentiation of allergens should always be carried out to develop a specific single treatment for the patient.
Screening tests with reaction class 1 result: Does it make sense to perform allergen differentiation or make ASIT?
If the screening test gives a reaction class 1, it is not predictable whether the subsequent differentiation will be negative or positive.
Given a compatible history and clinical picture is always advisable to carry out allergen-specific immunotherapy even with reaction class 1 results, especially when the results are correlated with the clinical and medical history.
Glucocorticoids: What are the withdraw times of topical, oral and depot corticosteroids for allergen testing? Do they also need to be applied when testing for food allergens?
Glucocorticoids are anti-inflammatory drugs that, depending on the dose, can have an immunosuppressive effect.
The use of glucocorticoids in allergy management must be restricted to low anti-inflammatory doses to control inflammation and pruritus.
Nevertheless, the use of high doses, long treatments or administration by several routes (e.g., oral and topical) can reach levels of immunosuppression.
Glucocorticoids have less influence on humoral immunity than on cellular immunity, and existing antibody levels are not usually reduced, but the production of new antibodies can be reduced. In our experience, we can see negative results in allergy tests associated with glucocorticoid treatments. So, our recommendation is to follow withdrawal times before serological allergy tests. You can switch to another antipruritic treatment prior to the allergy test (e.g. lokivetmab).
Our extended withdrawal times are proposed for the worst case scenarios, every case must be individually evaluated.
Proposed withdrawal times to minimise the risk of false negative results associated with treatment
• Local/topical corticosteroids: 2-4 weeks.
• Oral corticosteroids (e.g. prednisolone): up to 8 weeks.
• Depot corticosteroids: up to 3 months.
It is possible to shorten the withdrawal time, but if the results are negative, we recommend to repeat the test after the proposed withdrawal times are completed.
Examples of treatment that don‘t imply a significant risk of negative results in allergy tests (but we never can guarantee that there is NO risk):
1. Use of topical hydrocortisone aceponate – withdrawal time 0
2. Five days of prednisolone at 0.5mg/kg daily
3. Prednisone/prednisolone 0.25mg/kg q48h
Each individual is different, and some animals still show high antibodies despite receiving long and high corticosteroid doses.
Some patients who receive therapy with eye drops or ear medication containing corticosteroids may have a reduced level of antibody production.
Glucocorticoid withdraw times are aplicable to all allergy tests, including food allergens since they measure levels of IgE and IgG antibodies.
Glucocorticoids: Is it possible to interpret a positive allergy test with previous cortisone treatment? Does this also apply to a negative result?
A positive result, even with previous corticosteroids intake, is always interpreted as positive. If the withdraw time had been respected, higher antibody values would be obtained.
On the contrary, a negative result may be false due to the immunosuppressive effect of corticosteroids. In these cases, the result is always in doubt, and it is advisable to carry out a new test respecting the withdrawal times of drugs.
Oclacitinib: Can this alter the results of allergy tests?
Several studies agree that Oclacitinib does not influence the results of allergy tests in the first four weeks of treatment. However we cannot find any studies relating to the possible effect of longer periods of treatments. We have seen some animals taking oclacitinib becoming completely negative in their allergy tests. If the results of the allergy test during oclacitinib treatment are negative, we recommend to repeat the test without the treatment and observe the withdrawal time.
Mites: The screening test shows positive results for mites. Does the animal have parasitic mites?
The screening test measures IgE levels against environmental mites (dust and storage mites).
A positive mite result in the pretest has nothing to do with ectoparasites!
Warning: There is cross-reaction between Sarcoptes scabiei and dust mites. In the case of sarcoptic mange, positive results can be obtained for dust mites.
Mites: How can dust and storage mites be prevented?
It is not possible to completly avoid contact with these mites, but it is possible to reduce the amount in the environment with some measures.
• Dust mites are found mainly in beds, upholstered furniture, and carpets. It is recommended that the animal sleeps on an antimite bed or mat, in a room without carpets and never in their owners bed. There are anti-mite sprays that can be applied at home.
• Storage mites are found in dry food storage, rice, cereal flakes, etc., but also in environmental dust. Wet feeding does not eliminate full contact with the mites. Conserve dry food in hermetic plastic packets.
Mites in food: Is it helpful to freeze the dry food to avoid the mites?
Freezing food prevents mite reproduction, but if they were there, their structural proteins would be preserved, so exposure to allergens is not avoided.
The contamination of food by mites depends mainly on its packaging and its storage. The feed should always be kept in dry places and in tightly closed containers that are not permeable to mites: plastic containers with zip closures or „tupperware“.
Feeding atopic animals: Can fruits and vegetables cause food or contact allergies (cross-reactions to pollen)?
Yes, it is possible. These phenomena are called cross-reactions (OAS = oral allergy syndrome). The individuals cannot only react to the already known allergy-causing allergen but can also show reactions to other substances that share similar protein structures (epitopes). When food and environmental allergens share similar molecular structures, cross-reactive IgE antibodies can be produced. The cross-reaction can occur between fruits or between fruits and pollens, making possible the development of food allergies associated with pollen.
In the so-called „fresh fruit syndrome“ in humans, the clinical signs of an allergy to birch pollen can be triggered by eating carrots or apples. In human medicine, such reactions are well documented, but there are scarce publications in veterinary medicine.
The oral allergy syndrome, from ingestion of fruits and vegetables, should be considered during elimination and provocation diet trials (see frequently asked questions about food allergies).
Feeding atopic animals: What is meant by the "fresh fruit syndrome"?
The „fresh fruit syndrome“, also known as oral allergy syndrome (OAS), is described in human medicine. It is related to cross-reactions between pollens (from birch, mugwort or grasses) and fruits (apples, peaches, pears, melons) or vegetables (celery, tomato). To avoid this process, peel and cooking these foods is helpful.